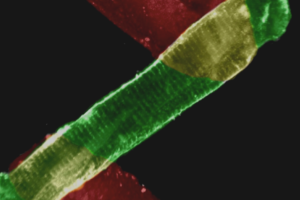
The control of Ca2+ influx and NFATc3 signaling in arterial smooth muscle during hypertension.
Nieves-Cintrón M, Amberg GC, Navedo MF, Molkentin JD, Santana LF
Abstract:
Many excitable cells express L-type Ca2+ channels (LTCCs), which participate in physiological and pathophysiological processes ranging from memory, secretion, and contraction to epilepsy, heart failure, and hypertension. Clusters of LTCCs can operate in a PKCα-dependent, high open probability mode that generates sites of sustained Ca2+ influx called “persistent Ca2+ sparklets.” Although increased LTCC activity is necessary for the development of vascular dysfunction during hypertension, the mechanisms leading to increased LTCC function are unclear. Here, we tested the hypothesis that increased PKCα and persistent Ca2+ sparklet activity contributes to arterial dysfunction during hypertension. We found that PKCα and persistent Ca2+ sparklet activity is indeed increased in arterial myocytes during hypertension. Furthermore, in human arterial myocytes, PKCα-dependent persistent Ca2+ sparklets activated the prohypertensive calcineurin/NFATc3 signaling cascade. These events culminated in three hallmark signs of hypertension-associated vascular dysfunction: increased Ca2+ entry, elevated arterial [Ca2+]i, and enhanced myogenic tone. Consistent with these observations, we show that PKCα ablation is protective against the development of angiotensin II-induced hypertension. These data support a model in which persistent Ca2+ sparklets, PKCα, and calcineurin form a subcellular signaling triad controlling NFATc3-dependent gene expression, arterial function, and blood pressure. Because of the ubiquity of these proteins, this model may represent a general signaling pathway controlling gene expression and cellular function.